*Disclaimer: This post is in no way intended to dissuade you or anyone from having a Bulletproof or Keto Coffee. I still have them daily, but after performing the Fat Tolerance Test (FTT) on myself, I've cut back on the amount of butter I used in my coffee–particularly on days when I'm not exercising shortly after ingesting the coffee.
Why You Should Consider a Fat Tolerance Test (FTT)
Getting routine blood work is like changing the oil in your car. It’s just something you have to do if you want your body—or your car’s engine—to thrive with time.
At present, most doctors suggest “fasting” before getting your blood work, especially lipids checked (e.g., triglycerides and cholesterol).
But most people are hardly ever in a fasted state—at least not on a routine basis.
OK, since you’re reading this, you likely have a compressed feeding window—wherein you fast for 12 to 16 hours a day—but food bookends most people’s day, and snacks, treats and desserts fill in the gaps.
So, when most folks get their “fasted” blood work, it’s not a true representation of how their blood actually looks in a truly fasted state. Many astute and well-intentioned health professionals rely on blood work as part their overall evaluation of health and disease processes.
Fasting is even more emphasized by practitioners when it comes to assessing commonly overlooked biomarkers, such as blood triglycerides and cholesterol.
Making the Case for Non-Fasted Lipid Testing
On a spring morning in 2011 while drinking coffee at INK! in Denver, I stumbled upon a consensus article that got me interested in the whole non-fasted blood testing idea. (Kolovou 2011)
I was surprised to learn that traditional clinical recommendations to test triglycerides in a fasted state have nothing to do with enhancing test accuracy or feasibility.
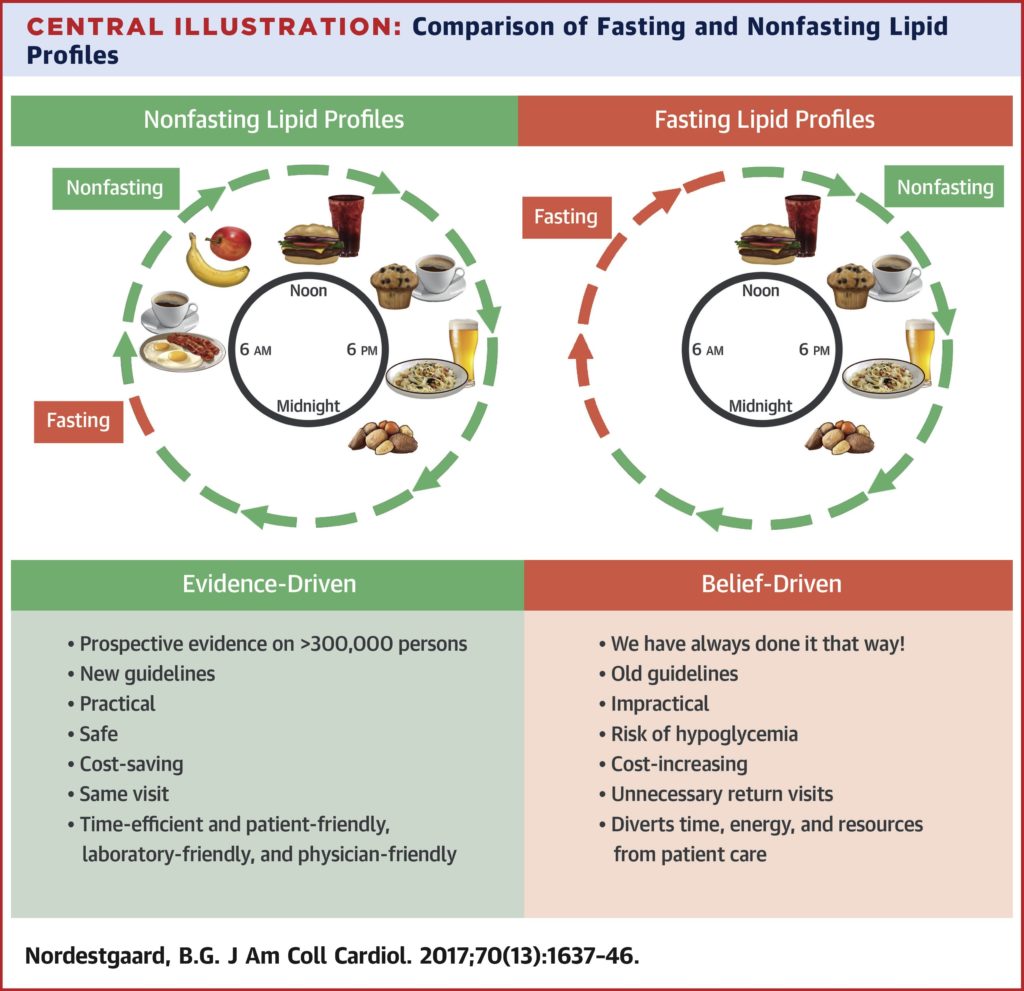
The two primary reasons why a majority of doctors suggest that you fast before blood work, especially lipid tests, are:
- Fasting minimizes major fluctuations in a patient’s triglyceride levels.
- LDL-C measurements used to be derived indirectly via the Friedewald equation for which fasting was necessary. (Now, most labs can directly measure LDL-C.)
It goes without saying that in 2018, there’s really no compelling clinical reason to continue to suggest fasting before testing blood triglycerides and cholesterol.
In fact, multiple studies suggest that elevated non-fasting triglycerides strongly and independently predict heart disease and stroke better than other commonly used biomarkers, like LDL-cholesterol.
A few of these large population studies associate elevated non-fasting triglycerides with cardiovascular events are the Women’s Health Study, the Physicians’ Health Study, the Northwick Park Heart Study, the Copenhagen City Heart Study and several others.
Previous studies showed that there is some difference in the predictive value of nonfasting triglycerides between men and women (1, 4, 5 ), as the results for men are somewhat less predictive than those for women (Langsted 2015)
In this studies, non-fasting triglycerides over 176 mg/dL or 1.99 mmol/L are associated with an increased risk of a heart attack and stroke. (It doesn’t mean that triglycerides cause heart disease, it’s just an association.)
Ideally one’s plasma triglycerides in the non-fasted state would be under 180 mg/dl, per an expert consensus panel.
Introducing the Fat Tolerance Test (FTT)
Doctors across the world utilize the glucose tolerance test (GTT) to assess diabetes risk in their patients. But glucose is just one energy substrate in the blood, and it’s increasingly becoming out of vogue.
Fat is back. (Since you’re likely a keto dietary, you already know this.)
We’ve assumed that because ingesting a dietary doesn’t raise insulin that it must be inert.
Bacon, butter, cream, bring it on!
But ingested fat is still energy, it’s got to be either utilized (burned as fuel) or stored as fat.
So why not stress-test your body with a load of lipids, say the 20+ grams of fat in a Bulletproof or keto coffee and see how your body responds.
Since my brother Kyle introduced me to Bulletproof coffees in 2012, I’ve been drinking them regularly and quite like them. (Thanks, Kyle!)
Since I know my fasting triglycerides have hovered right around 60 mg/dL for the past 10 years—event after going keto in 2015—I figured why not test how my body metabolizes this popular coffee drink?
To “stress-test” my lipids, I followed the recommendations provided in the consensus paper listed below, with a slight modification.
The expert panel suggest eating a mixed meal consisting of 75 grams of fat, 25 grams of carbohydrates, and 10 grams of protein and measuring blood triglycerides four hours after the meal.
Since I normally don’t eat that much fat, with that little protein and moderate carbs, I decided to tweak things that would be more representative of something I usually eat.
On non-training days I usually have a Bulletproof coffee—1 heaping tablespoon of butter mixed with one tablespoon of MCT oil—and I’ll snack on a handful of nuts. Usually Brazil, pecans or sprouted walnuts.
90 minutes prior to getting my labs drawn last February, I had my Bulletproof coffee and a few nuts as usual.
I had my labs drawn about two hours later. To my surprise, having a “keto fatty coffee” shot my triglycerides up 216 mg/dL. I was expecting a rise in triglycerides, but didn’t think I’d shoot over 200 mg/dL.
The desirable non-fasting triglyceride level after the FTT deemed healthy by the expert panel is anything less than 220 mg/dL or under 2.5 mmol/L.
Anything over that is considered undesirable postprandial lipemia. (Phew…I can still fuel my fatty coffee addiction!)
Limitations of My First Fat Tolerance Test (FTT)
This was my first test, and the lipid load was only ~ 50 grams of fat. I plan to repeat the test using at 70 gram of fat test meal.
Related Content:
References
(Kolovou 2011) Kolovou, G. D., Mikhailidis, D. P., Kovar, J., Lairon, D., Nordestgaard, B. G., Ooi, T. C., et al. (2011). Assessment and clinical relevance of non-fasting and postprandial triglycerides: an expert panel statement. Current Vascular Pharmacology, 9(3), 258–270.
(Langsted 2015) Langsted, A., & Nordestgaard, B. G. (2015). Nonfasting Lipid Profiles: The Way of the Future. Clinical Chemistry, 61(9), 1123–1125. http://doi.org/10.1373/clinchem.2015.243139
(Nordestgaard 2017) Nordestgaard, B. G. (2017). A Test in Context: Lipid Profile, Fasting Versus Nonfasting. Journal of the American College of Cardiology, 70(13), 1637–1646. http://doi.org/10.1016/j.jacc.2017.08.006
(White 2015) White, K. T., Moorthy, M. V., Akinkuolie, A. O., Demler, O., Ridker, P. M., Cook, N. R., & Mora, S. (2015). Identifying an Optimal Cut Point for the Diagnosis of Hypertriglyceridemia in the Nonfasting State. Clinical Chemistry, 61(9), clinchem.2015.241752–1163. http://doi.org/10.1373/clinchem.2015.241752

Hi Mike,
I’m also into coffee with butter or coconut oil. Coconut oil is perfect and I take it 15gr. into coffee but man I thought you knew this… you cannot eat with your coffee Mike bc this is not good for your cortisol. The fat in BP is only there for step by step release of the caffeine. I do not eat until 13-14h and in the morning I take only 25gr. Protein (whey+gelatin), 10gr. of red palm-oil with some stevia and then I make a cup with a lot of thee-herbs in it and there I put the coffee in with 15gr. of fat. Not more and works great and then around 11h I take another herb-coffee with fat and then around 13-14h I have my lunch but after that no coffee. Just green tea with some fats. But what I want to say is do your test with less fat and no other foods with the coffee. Is to much calories in the morning and your blood sugar is also higher in the morning so the extra cortisol and calories you can miss.
Test it out
Kevin z. from Belgium
HI there,
The fat in the coffee is intended to enhanced ketogenesis in the liver. Purpose of this test, the Fat Tolerance Test (FTT) was to see how my body responded to a lipid load.
The expert panel listed above suggests 50 to 70 grams of lipids and testing blood triglycerides in the four hour window after.
Thanks!
Mike
I love this. Does this work the same in regards to fasting with metabolic panels?
Akemi
Hi Akemi,
This is a great question. Potentially, but the data is just now emerging re: lipid testing in the non-fasted state–at least as an option to see how the body is tolerating lipid loads in the post-meal window!
Worth looking into for certain clients/patients,
Mike